Patellofemoral pain syndrome (PFPS) is one of the most common knee conditions. It affects both the young active sportsperson and the elderly. It usually signifies pain felt behind the kneecap, where the patella (kneecap) articulates with the lower end of the thigh bone (femur). This joint is known as the patellofemoral joint.
Patellofemoral pain affects 1/4th of the normal population at some point of time in their lives but it is more common in athletes. Patellofemoral pain syndrome is typically seen in sports that require running, jumping, and landing or squatting position is required.
If PFPS is left untreated for some time it can predispose the person to “patellar tendinitis”.
Causes of Patellofemoral Pain Syndrome
Patellofemoral pain syndrome is mainly due to poor kneecap alignment and maltracking while bending and extending the knee resulting in excessive intrarticular pressure in the patellofemoral joint. Repeated trauma as a result of maltracking causes an increase in retro patellar joint forces, which can lead to kneecap pain, joint irritation, and eventually degeneration of patella joint surface.
The common causes of patellar malalignment are
- Muscle imbalance and
- Poor biomechanical control.
- Causes of Muscle Imbalance,
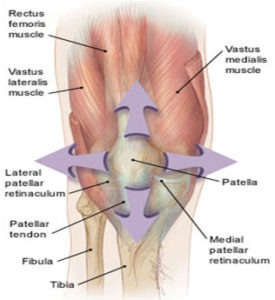
Patella is basically a sesamoid bone that lies within the quadriceps muscle and is attached to the shin bone through the patellar tendon.
The muscle imbalance that usually occurs is between the vastus lateralis (VL), which pulls the patella up and outwards, and the vastus medialis obliquus (VMO), which pulls the patella up and inwards. As the outer forces predominate, causing the patella to track laterally in the groove.
VMO helps is a terminal extension of the leg which is normally a passive process in normal individuals except athletes so it gradually undergoes atrophy. As a result, lateral forces predominate and laterally pull the patella causing mall tracking of patella during knee movements. In athletes, injury to knee/ surgeries around the knee may predispose patellar mall tracking.
The tightness of lateral knee structures (lateral retinaculum, Vastus Lateralis, and Iliotibial Band) will cause the patella to shift laterally over time.
Hip muscles have been shown to be very important in the control of knee. Poor buttock muscle control causes knee to roll in and apply a relative lateral displacement of the patella. Most successful rehabilitation programs require assessment and correction of hip and buttock muscle control.
- Cause of poor biomechanical control
Poor foot posture (e.g. flat feet) and weak hip control muscles can both allow the knee to abnormally twist and result in a lateral deviation of the patella. When poor biomechanics are repeated with each step of walking or running pattern, it traumatizes the patellofemoral joint causing pain.
Symptoms of Patellofemoral Pain Syndrome
The onset of pain is gradual.
Pain is normally felt during weight-bearing activities that involve knee bending.
Activities that involve repetitive knee bending like stair climbing, squatting, kneeling, hopping, running are commonly painful.
As the syndrome progresses knee becomes more painful with movement and pain may be felt without movement as well.
Pain may appear on prolonged sitting (sustained knee bending) especially on chairs with a higher edge than the base. A nickname for this condition is “theatre knee”.
Treatment of Patellofemoral Pain Syndrome
Physiotherapy treatment has proved to be very effective short and long-term solution for PFPS.
Approximately 90% of patients with PFPS will be pain-free within six weeks of a Physiotherapist-guided rehabilitation program.
For those who fail to respond, surgery may be required to repair associated injuries such as severely damaged or arthritic joint surfaces.
The short-term aim of treatment is to reduce pain and swelling and then, more importantly, correction of the cause to prevent it from reoccurrence in the long term.
There is no specific time frame for when to progress from each stage to the next. The injury rehabilitation will be determined by many factors during physiotherapist’s clinical assessment.
The physiotherapist may seamlessly progress between the rehabilitation phases as the clinical condition of the patient improves. It is also important to note that each progression must be carefully monitored as attempting to progress too soon to the next level can lead to re-injury.
Phase 1 – Injury Protection: Pain Relief & Anti-inflammatory Tips
As with most cases of soft tissue injuries the initial treatment is – Rest, Ice, and Protection.
- Rest: In the early phase the best is to avoid all activities that induce pain.
- Ice is a simple and effective modality to reduce pain and swelling. Apply ice for 10-15 minutes every 2 to 4 hours during the initial phase.
- Protection: the physiotherapist may normally apply supportive taping or crepe bandage to help relieve pain and commence the patellofemoral joint realignment phase. The patellofemoral taping is normally immediately effective in providing pain relief.
The physiotherapist may utilize a range of helpful tricks including pain-relieving techniques, joint mobilizations, massage, and strapping to assist during this painful phase.
Anti-inflammatory medication and creams may help reduce pain and swelling.
Phase 2: Regain Full Range of Passive Motion
The patella and knee must be able to glide through its full normal range of motion. A physiotherapist will assess the motion and apply the necessary techniques to normalize joint range of motion.
Phase 3: Restore Full Muscle Length
The hamstring and calf muscles are stretched is they are tight and are causing excessive tension or pressure on the patella. It is important to regain normal muscle length to improve lower limb biomechanics.
Phase 4: Normalize Quadriceps Muscle Balance
In order to prevent a recurrence, quadriceps muscle balance and its control should be assessed properly by a physiotherapist. In most instances, patients will require a specific knee strengthening program.
Phase 5: Normalize Foot & Hip Biomechanics
Patellofemoral pain syndrome can occur from poor foot biomechanics (e.g. flat foot) or poor hip control.
In order to prevent a recurrence, the foot and hip control should be assessed properly by a physiotherapist. In some instances, the patient may require a foot orthotic (shoe insert) or Active Foot Posture Stabilization program. Other patients may require a hip stabilization program.
Phase 6: Normalize Movement Patterns
Patellar pain commonly occurs from a poor or abnormal gait, jumping, landing, running or squatting technique. In order to prevent a recurrence, the walking pattern, jumping and landing technique, running style or squatting method should be assessed and corrected as required.
Phase 7: Restore High Speed, Power, Proprioception and Agility
Most patellofemoral pain sufferers need to return to high speed or repetition activities, which place enormous forces on the knee. The physiotherapist can guide an athlete properly how to return to sports planning.
Balance and proprioception (the sense of the relative position of neighboring parts of the body) are both known to be adversely affected by patellofemoral pain. To prevent a re-aggravation, both aspects need to be assessed and retrained.
Depending on what the sport or lifestyle entails, a speed, agility, proprioception and power program will be customized to prepare for light sport-specific training.